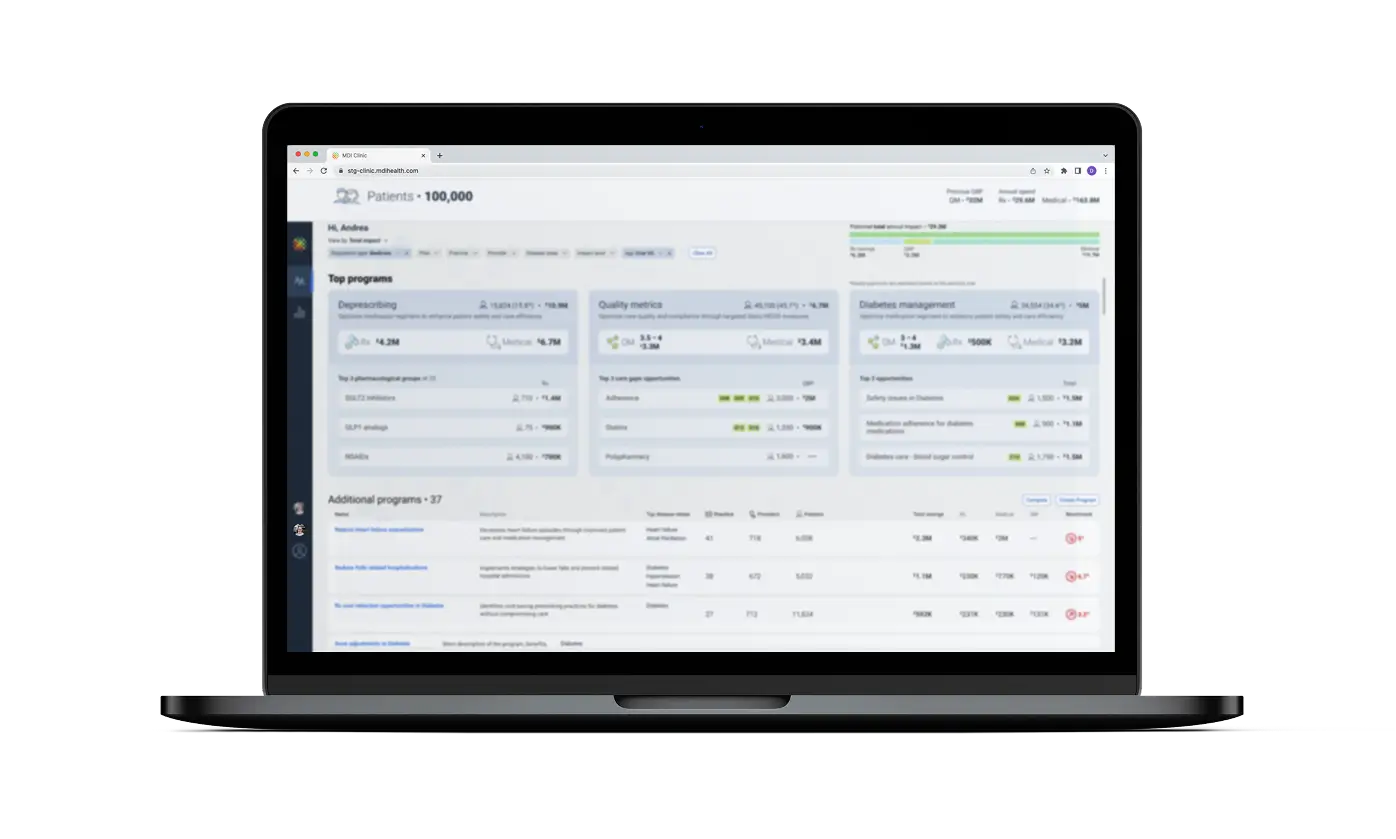
Quality Improvement
Boost STARs & Quality Measures
- Discover underlying non-adherence issues through automated clinical analysis
- Harness real-time analytics that flags urgent quality gaps and tracks outcomes
- Use our identification tool to see which patients are at risk of becoming non-adherent
- Deliver interventions that boost quality measures while reducing cost of care
10X Efficiency
In case reviews
11+ Measures
STARs and Other Quality Metrics
$2,000 PMPY
In Rx & medical savings
AI Medication Management Platform Optimizing STARs & Quality Metrics
Prioritization Based on Care Gaps, Timing & Costs
Utilize our customized prioritization & programs to see interventions based on quality needs such as timing, quality measure, clinical urgency, opportunity for additional cost reduction interventions and more

Predicting Nonadherence & Its Clinical Drivers
MDI identifies patients at risk of becoming non-adherent and highlights the underlying clinical reason for non-adherence, allowing care teams to be more targeted and efficient when reaching out to patients

Personalized & Scalable Quality Interventions
MDI goes beyond generic care gap alerts by providing actionable & personalized ready-to-send recommendations to close care gaps more efficiently

Clinically-Based Quality Recommendations
Care gaps recommendations include patient specific clinical context, using patients’ demographics, conditions, medical history, labs and more, to suggest highly accurate & actionable interventions
Increasing Gap Closure Through Consolidated Engagement
Manage quality and cost containment programs in one platform, prioritizing the most urgent interventions across the programs, while consolidating outreach with all the urgent interventions to minimize outreaches and maximize impact

Customized Analytics & Dashboards
Create tailored programs and assign patient cases based on urgency, quality measures, provider, timing, clinical risk, and more. Monitor progress and outcomes including adoption, care gap closure, and program impact.
Example Quality Measures MDI Impacts:
Medication Adherence for Diabetes Medications
Medication Adherence for Hypertension
Medication Adherence for Cholesterol
Statin Use in Persons with Diabetes
Concurrent Use of Opioids and Benzodiazepines
Polypharmacy Use of Multiple Anticholinergic Medications in Older Adults

The Most Comprehensive Patient Analysis, at Scale
Population & Patient Data
Hospitalizations
Labs and test values
Demographics and member enrollment data
Medications (current and past) & refill date, dosage
Conditions (current and past)
Provider specialty, clinics, networks & locations
MDI Sourced Data
Pharmacological & medical literature
CMS and rolling basis Adherence information
CMS STARs, HEDIS & PQA guidelines
Clinical guidelines (ADA, AHA, AGS, and more)
FDA guidelines & prescribing information
Medical codes
Example User Workflow
Data feed
from client
View population dashboards highlighting quality gaps by urgency and need
Select customized programs based on KPI’s
Assign MDI’s programs to pharmacists
Prepared patient analysis & ready-to-send recommendations
Recommendations sent to providers/members based on configuration and workflow (EHR, internal system, etc)
Track adoption, care gap closure and STARs impact predictions via MDI’s dashboards
Customized reporting on operational, clinical & financial outcomes
Discover How MDI Can Improve Your Quality Ratings, Optimize Clinical Outcomes, and Reduce Costs by ~$2,000 PMPY